Hair infection from fungal agents, also called trichomycoses, is one of the common concerns in humans. Fungi or fungus are single celled or multinucleate organisms that decay and absorb the organic material in which they grow (including yeasts, mushrooms, molds, smuts, rusts and mildews). There are three common agents causing hair infections:
- Dermatophytes
- Malassezia infections
- Piedra
Through a series of blog posts, we will take a deeper look at each type of fungal scalp infection, including the most common diseases impacting the hair follicle.
Dermatophytes
Dermatophytes are fungi that require keratin for growth. These fungi directly invade when conditions are prime for habitation and can cause superficial infections of the skin, hair, and nails.

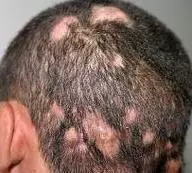
Tinea Capitis or Ringworm
The dermatophyte Tinea Capitis, otherwise known as ringworm, is the most common fungal infection of the scalp. According to the world heath organization, it accounts for more than 90% of fungal infections in Europe and the Americas.
This infection is actually a fungus, not a worm. If you have ever suffered from a bout of athlete's foot, you've suffered from the same fungus. Ringworm gets its name from the ring-like shapes that form and become visible on the surface of the skin, and when the scalp is affected, patchy hair loss is quite common.
Symptoms of the Infection
- The first sign is usually the presence of a small pimple that expands.
- Usually, the infection just looks like severe itchy dandruff on various places on the scalp, which may be confused for psoriasis.
- The natural reaction is most likely to be scratching, leading to hair loss.
- As the fungus spreads into hair fibers, hair becomes brittle and breaks off resulting in a scaly bald patch.
- Bald patches could also become painful, blister, ooze, and boils (pustules) can develop on the scalp. If not prescribed early, this can cause permanent scarring and hair loss.
- Some severe infections may produce a fever, and the glands could swell in the neck.
Diagnosing the Infection
A visual exam is often enough to diagnose ringworm of the scalp. A skin or hair sample could be taken to confirm the diagnosis. The sample of your hair or a scraping from a scaly patch of the scalp is viewed under a microscope to determine the presence of fungi.
Contracting the Infection
From Person to Person
- Most cases of scalp ringworm are passed from person to person by touching, sharing towels, etc.
- Some people are just carriers of the fungi. Meaning the fungi on their skin and hair does not cause symptoms or infection. However, they could pass the fungi on to others who then develop symptoms.
- Fungi and their spores can also survive on combs, brushes, unwashed towels, furniture, and sheets for long periods.
- An outbreak of scalp ringworm can occur in schools or families.
From Animals
- Some cats, dogs, and other pets have fungal infections on their skin, and they could pass the infection on, particularly to children. (Animals can be treated by your vet.)
- Cats or dogs (especially kittens and puppies) or other animals (such as cows, guinea pigs, and other animals) may be reservoirs for infection.
- The animals can have clinical signs of dermatophyte infection with scaling and hair loss, but can also be carriers and show no symptoms.
- Farm animals could also be a source, and just touching a farm gate where infected animals pass through may be sufficient to infect your skin.
No Apparent reason
- Fungi are common, and infection can appear 'out of the blue.'
- For example, fungal spores can simply get into the air from an infected person and land on the scalp of another person. The spores may then progress into fungi and cause infection.
Ringworm Treatment
Medical Treatment
- Use a shampoo with antifungal properties (selenium sulfide 1 or 2.5%, ciclopirox 1%, or ketoconazole 2% shampoo) at least twice weekly to decrease shedding of fungal spores.
Reduce Spread and Recurrence
Person to Person
- Members living in the house of an individual diagnosed with ringworm should be physically examined for signs, and treated simultaneously if ringworm is detected.
- HOWEVER even those showing no symptoms may be carriers of dermatophytes and serve as reservoirs for recurrent infection.
- Because of this possibility, an antifungal shampoo by all household members should be used for two to four week to decrease rick of reinfection. Household members should begin to use the shampoo when the infected individual begins treatment for tinea capitis.
In Children
- Children with tinea capitis should avoid sharing hair care tools and headwear (helmets or hats) with other people.
- Participation in sports with heat-to-head contact should be avoided.
In the House
- Pillowcases should not be shared.
- Bedding and towels used by the infected individual should be washed. Wash towels after each use. Furniture that is frequently in direct contact with the affected person or pet should be washed if possible.
- It is also recommended that combs and hair trimming equipment be cleaned mechanically and disinfected (with household bleach), soak combs and brushes in a mixture of one-half bleach and one-half water.
- If there is an outbreak of tinea in a family, the pet (especially if new) should be evaluated by a veterinarian. The animal should also be assessed if the patient or other household members experience recurrent dermatophyte infections.
Ringworm can resemble other scalp conditions, which may not prompt cause for alarm, but this fungal infection is highly contagious. It’s important to get it under control and stop any potential spreading as soon as possible. Generally if ringworm is treated effectively and early enough, hair loss is not permanent. For more information on how to win the battle with hair loss regardless of the cause, please contact us at HT&RC for a consultation.